Shelby Nursing Home Abuse Lawyer

Cleveland County is rural North Carolina, and rural means something specific when it comes to nursing home care. It means fewer facilities, fewer qualified nurses willing to work in those facilities, and fewer alternatives for families when the one local nursing home is not providing adequate care. Shelby is the county seat of a county where the nearest major hospital system is forty minutes away in Gastonia or Charlotte, where the pool of CNAs and LPNs is small and getting smaller, and where a single nursing facility’s staffing decisions can affect the safety of a disproportionate number of the county’s elderly residents. The rural nursing home crisis is not an abstraction in Cleveland County. It is a daily reality that puts vulnerable people at risk.
Ryan Duffy evaluates nursing home neglect claims for Cleveland County families at no charge. If your loved one has been harmed in a Shelby-area facility, the Law Office of Ryan P. Duffy will review the situation and connect you with attorneys who understand the particular challenges of litigating nursing home cases that arise in rural communities.
Extreme Staffing Shortages in Cleveland County: A Crisis With Consequences
The staffing crisis in rural nursing homes is a self-reinforcing cycle. Facilities in Shelby and Cleveland County cannot match the wages or benefits offered by hospitals and nursing homes in Charlotte, Gastonia, or Asheville. As qualified workers leave for better-paying positions, the remaining staff are forced to cover more residents per shift, increasing their workload and accelerating burnout. Burnout leads to more departures, which leads to more overtime for those who remain, which leads to more burnout. The cycle continues until the facility is operating at staffing levels that make adequate care mathematically impossible.
In a properly staffed facility, one CNA typically cares for eight to ten residents during a day shift. In understaffed Cleveland County facilities, a single CNA may be responsible for fifteen, eighteen, or even twenty residents. At that ratio, there is not enough time in an eight-hour shift to provide each resident with the basic care they require: bathing, toileting, repositioning, meal assistance, and responding to call lights within a reasonable time. Something has to give, and what gives is the resident’s dignity, comfort, and safety.
The consequences are predictable and documented. Residents develop pressure ulcers because they are not being repositioned on schedule. Residents fall because call lights go unanswered and they attempt to transfer or ambulate without help. Residents become dehydrated and malnourished because there are not enough aides to assist with meals and fluid intake. Residents sit in soiled clothing because the aide cannot get to them fast enough. Each of these outcomes is a direct result of a staffing level that the facility chose, and each is a basis for a negligence claim under North Carolina law.
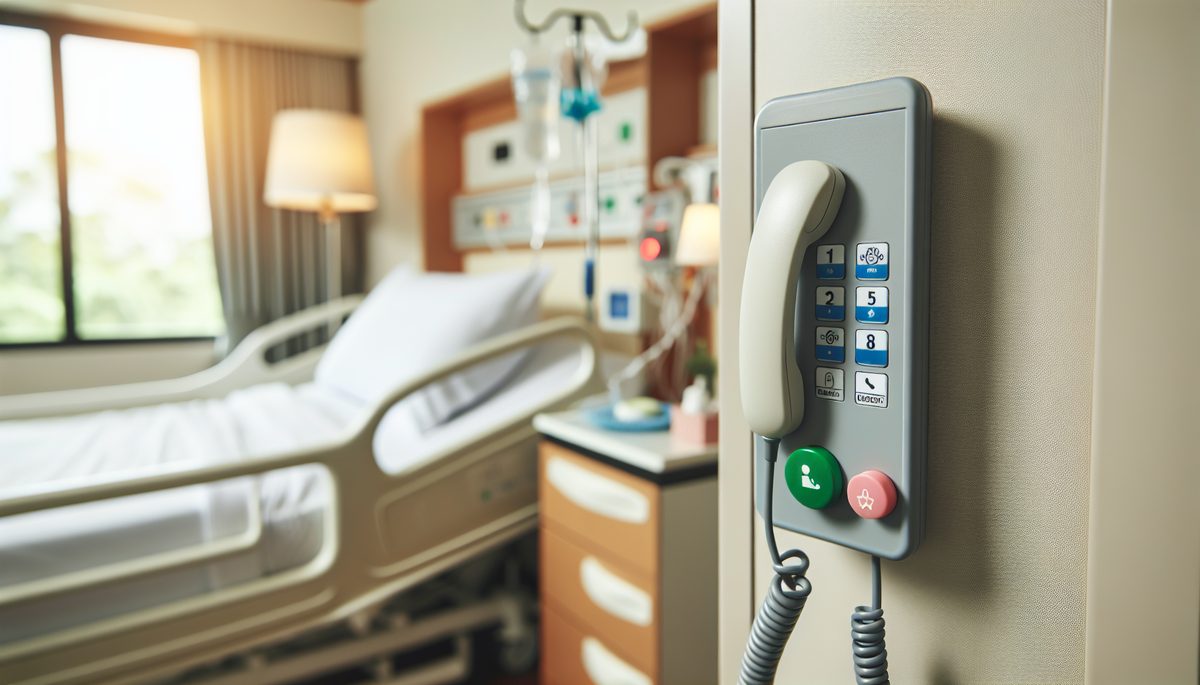
Emergency Preparedness Failures in Rural Facilities
When a medical emergency occurs at a Shelby nursing home, the response time for ambulance and emergency medical services is significantly longer than what a family would expect in Charlotte or even Gastonia. Atrium Health Cleveland in Shelby is the closest hospital, but depending on the location of the facility and the severity of the emergency, a transfer to a larger hospital in Gastonia or Charlotte may be necessary, adding another thirty to forty-five minutes of transport time. This geographic reality places an additional obligation on the facility to have robust emergency preparedness protocols.
A facility that knows its residents are thirty minutes or more from definitive hospital care must maintain trained staff who can provide effective first response, stabilize a resident experiencing a medical emergency, and initiate appropriate interventions before EMS arrives. When a resident has a stroke and the overnight shift aide does not recognize the symptoms, when a resident goes into cardiac arrest and no staff member on duty is current on CPR certification, or when a resident aspirates during a meal and no one is trained in airway management, the delay between the emergency and the arrival of paramedics becomes a period of preventable deterioration.
Rural facilities also face challenges during severe weather events. Power outages, road closures, and staffing absences during winter storms or hurricanes can leave facilities operating with skeleton crews and no backup power for extended periods. A facility that does not maintain a functional emergency generator, that does not have a severe weather staffing plan, or that does not have adequate medication and supply reserves for emergency conditions is endangering its residents. Cleveland County families should ask about emergency preparedness plans during the facility selection process and should not accept vague assurances.
North Carolina Legal Protections for Cleveland County Residents
The Nursing Home Patients’ Bill of Rights (N.C. Gen. Stat. 131E-117) requires facilities to provide adequate and appropriate care, which includes maintaining sufficient staff and having systems in place to respond to medical emergencies. A facility that cannot demonstrate it had adequate staff to meet its residents’ care plan requirements has violated this statutory duty. The contributory negligence defense is rarely applicable in staffing-related cases because the resident has no control over how many aides the facility schedules.
The statute of limitations is three years for personal injury and two years for wrongful death. In emergency preparedness cases where a delayed response contributed to a resident’s death, the wrongful death deadline is particularly important because these cases often involve rapid deterioration and death within days or weeks of the triggering event. Punitive damages may be available when the facility knowingly operated with staffing levels it knew were insufficient, or when it failed to maintain basic emergency response capabilities despite being aware of the risks posed by its rural location.

What Cleveland County Families Can Do
Request the staffing schedule for the facility and compare the number of CNAs and nurses per shift against the number of residents. Ask the facility how it handles medical emergencies, including who on staff is CPR certified and what equipment is available. Ask about the facility’s backup power supply and severe weather plans. During visits, observe staffing levels firsthand and note how quickly call lights are answered. Document any concerns with photographs and written notes. File complaints with NC DHSR at 1-800-624-3004. Contact an attorney to evaluate whether the facility’s staffing and emergency preparedness meet the legal standard of care.
How Ryan Duffy Serves Cleveland County Families
Ryan understands that families in rural areas often feel they have limited options. The closest alternative facility may be in another county, and the emotional and logistical toll of moving a loved one is significant. That reality does not excuse a facility from meeting its legal obligations. Ryan evaluates nursing home claims for Shelby and Cleveland County families at no charge and connects them with litigation attorneys who will hold the facility accountable regardless of how limited the local alternatives may be. There is no cost for the evaluation or referral.
Frequently Asked Questions
Can ambulance response time be used as evidence of negligence in a nursing home case?
The ambulance response time itself is not the facility’s fault, but it is relevant evidence. A facility that knows it is located in an area with longer EMS response times has a heightened duty to maintain staff trained in emergency response and to have appropriate equipment on hand to stabilize residents while waiting for paramedics. If the facility failed to initiate basic life-saving measures during the wait for EMS, and that delay caused or contributed to the resident’s death or worsened outcome, the facility’s failure to prepare for foreseeable emergency response delays supports a negligence claim.
What are the CNA-to-resident ratio standards in North Carolina?
North Carolina does not mandate specific CNA-to-resident ratios. Instead, the state requires facilities to maintain staffing levels sufficient to meet the needs documented in residents’ care plans. While there is no fixed number, industry standards and nursing experts generally consider a ratio of one CNA to eight or ten residents during the day shift and one CNA to twelve or fifteen residents during the night shift to be the minimum for adequate care. Facilities that operate with significantly higher ratios than these benchmarks are vulnerable to negligence claims supported by expert testimony.
Do families have the right to make unannounced visits to a Shelby nursing home?
Yes. Federal regulations guarantee residents the right to receive visitors, and North Carolina law reinforces this right. Families have the right to visit at any time of day, including evenings, nights, and weekends. The facility cannot restrict visiting hours to the point that families can only visit during times when staffing is at its highest and the facility is putting its best foot forward. Unannounced visits, particularly during evening and overnight shifts, are the most effective way to assess the actual quality of care your loved one is receiving.
Concerned About a Loved One? Free Case Evaluation
The Law Office of Ryan P. Duffy evaluates nursing home abuse and neglect cases and connects you with specialized attorneys at no additional cost.
Call us at 704-741-9399 or contact us online to get started.
The information on this page is for general educational purposes and does not constitute legal advice. Every case is different. Past results do not guarantee future outcomes. Contact our office for a free consultation to discuss the specifics of your situation.
Related Pages
Explore nearby pages for this city and practice area.

